How Technology Can Improve Home Care Staffing and Productivity Challenges
Healthcare industry pundits may have different perspectives about the next five to 10 years. But most agree about one crucial topic – the critical staffing shortage we’re already experiencing is going to get worse and will be magnified by more workers leaving the field.
A recent survey completed by Transcend Strategy Group showed that burnout is a major cause of healthcare workers leaving or wanting to leave their jobs within the next two years.
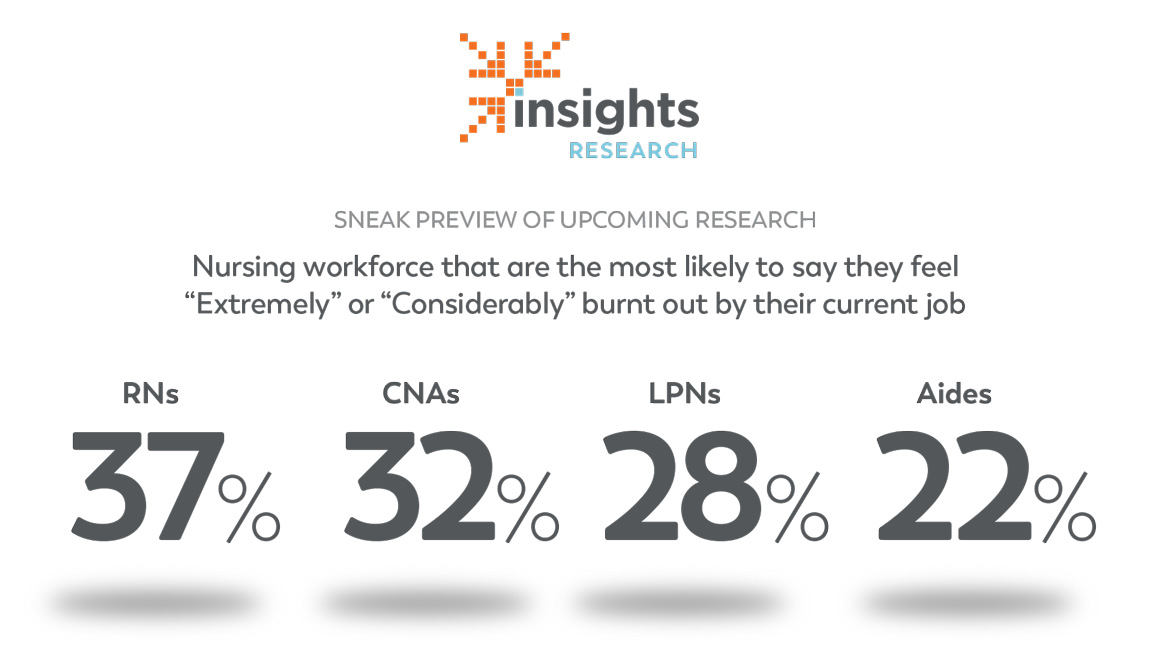
A sneak preview of the report shares this information:
“The majority of RNs report significantly higher levels of burnout compared to the rest of the nursing workforce. They are the most likely to say they feel ‘Extremely’ or ‘Considerably’ burnt out by their current job (37% vs. 32% CNAs, 28% of LPNs and 22% of Aides).”
If providers aren’t able to fill all their open positions, and they can stretch their remaining staff only so far without sacrificing quality, then another solution is sorely needed. That solution – or a big part of it – is technology.
Many of our home care clients bristle at first with the notion of ramping up technology in such a personal business. Technology and Artificial Intelligence are rapidly gaining in their capabilities, but they’re still not able to “read the room” and express compassion and empathy the way humans can. Emotional support for patients and families coping with serious illness will always be an invaluable part of what providers deliver every day.
I’m not suggesting that Rosie the Robot (who among our readers is old enough to remember The Jetsons?) should become Rosie the RN and replace nurses in the workforce. But I am definitely suggesting that technologies including telehealth, remote patient monitoring and reliable AI for production efficiencies MUST become a growing part of the answer.

What’s the right role for technology?
The COVID pandemic and isolation policies ushered in a surge of usage and acceptance of telehealth visits – particularly video chats replacing face-to-face appointments. In fact, Medicare added over 100 CPT and HCPCS codes for “the duration of the COVID-19 public health emergency.” A portion of those codes remain in effect.
Video chats are still a very useful tool in the telehealth toolbox, but they’re only scratching the surface. In addition to seeing patients’ faces and demeanor via video, the cameras on today’s devices can be a window to so much more. Clinicians can use the cameras as their eyes to check on matters such as wound care, edema, pressure sores and other issues that can be assessed visually. Family caregivers also can use the cameras to see demonstrations and instructions from clinicians on proper caregiving techniques.
Of course, the convenience and efficiencies of being able to perform such functions through video instead of clinicians having to drive to see the patient/family (or vice versa) are big advantages. Imagine the ability of clinicians to care for more patients efficiently if they didn’t have to deal with big chunks of windshield time throughout their day.
Beyond the video tools, however, telehealth includes so much more. One area that continues to grow is the toolbox for remote patient monitoring.
Monitoring vital signs remotely by clinicians can be crucial for catching warning signs early and preventing costly ER visits, which often lead to even more costly hospital admissions and readmissions.
In addition, remote monitoring of a change in condition could flag medication non-compliance – which is currently the number one cause of ER visits. (Ironically, this situation may not appear on the ER’s diagnosis report, but it’s the root cause of the diagnosis.)

The exciting usage and potential for remote patient monitoring
A growing selection of technology platforms and apps for remote patient monitoring continue to emerge in the market. Functionalities differ, but most depend on the patient, or more likely the family caregiver, to input information into the platform. An app may remind users that it’s time to take blood pressure, for example, and then request the results to be entered.
Ideally, the app is also linked with HIPAA-compliant encryption to the patient’s EMR, so data entry doesn’t have to be repeated. Syncing other platforms that are outside the EMR platform is often a big challenge … and one major area that the technology providers need to collaborate on more closely for the greater good of patient care.
An even better scenario involves technology that doesn’t require patient or family input, eliminating objections of “my mom doesn’t know how to use technology” and reducing the potential for data entry errors.
One type of product already on the market is a series of passive infrared sensors (called PIRs in the industry) placed strategically throughout the home. These sensors can discretely monitor the daily movements and habits of seniors to track normal patterns and note when behavior deviates from the norm. In addition to the sensors, AI comes into play in recognizing trends and deviances. AI can help connect the dots to note when something seems amiss. For example, a PIR can track how many times dad enters the bathroom. If there’s an excessive number of visits, it could be a warning sign of a UTI or digestive issue.

Even more exciting is the emerging connectivity of smart wearables and in-home medical devices. Items such as smartwatches are already monitoring vitals such as pulse, body temperature, blood pressure and blood oxygen levels. If a loved one is averse to wearing a smartwatch, a growing number of digital devices such as thermometers, blood pressure cuffs and blood oximeters are starting to incorporate Bluetooth connectivity.
Ultimately, the goal is to have these digital devices connect directly to the patient’s clinical team and, better still, their EMR to automatically log the data with no human input required.
What’s needed going forward?
The industry still has a way to go to bring this type of efficiency into everyday reality. I talked with a couple of technology providers, and heard general consensus on these areas that need to be further developed:
- Reliable and sustainable accuracy of wearables and home medical devices – Right now, the precision of digital home medical devices is all over the lot. Manufacturers could benefit by having a certification program with a “seal of approval” attesting to a device’s accuracy.
- Built-in Bluetooth connectivity to automatically send readings to clinicians or patient charts without technical proficiency or input required by patients or family caregivers (to reduce reporting errors). Both the sending and receiving platforms must have HIPAA-compliant safeguards.
- Data collection and communication platform – Ideally, this platform would combine the patient’s EMR with a HIPAA-compliant texting feature for easy communication between the clinical team and patient/family. Having a single, reliable repository for all patient data that can be accessed instantly by approved parties is a must (and what the EMR should be providing anyway).
- Clinician availability and training for prompt review of data – Since a big part of the goal of remote patient monitoring is to catch warning signs early, the system needs a clinician trained in the platform to check data at timely intervals throughout the day. Again, imagine the efficiency and productivity of a single clinician monitoring multiple patients from a single location.
How is your agency using technology? What are your plans for technology’s role in your future? Do you have the infrastructure and training programs to enable technology to take on a bigger role? Can you point to your technology as a differentiator for convenience, cost-efficiency and increased quality of care?
If you need help in thinking through a strategy for technology’s role in your organization, we’d love to be a part of that discussion. To start the conversation, email me at stan@transcend-strategy.com.










